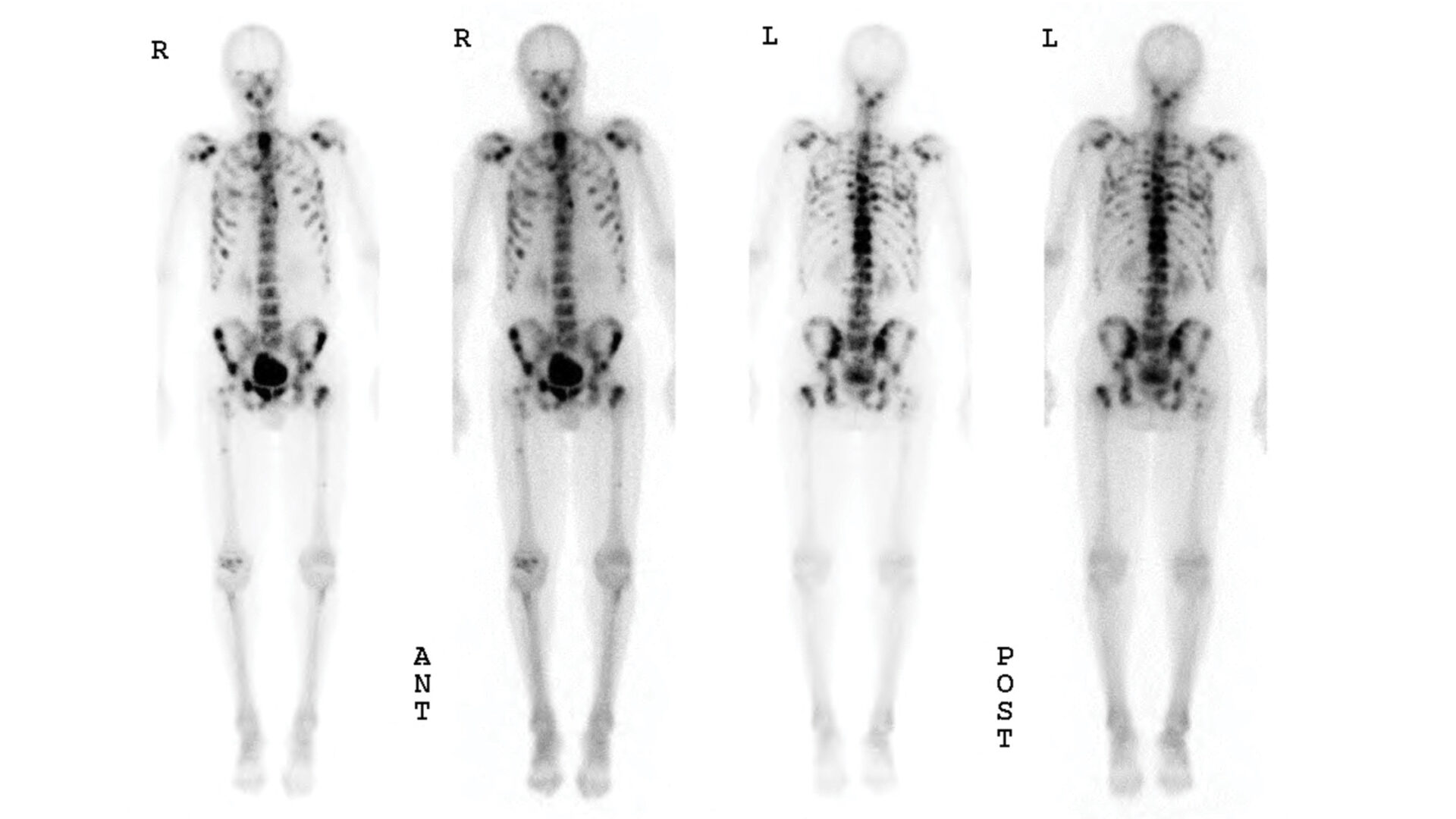
Referral Notes:
- Guideline-discordant imaging is common in staging patients with low-risk prostate cancer.
- In a stepped-wedge, cluster-randomized trial, NYU Langone Health researchers demonstrated that a physician-focused behavioral intervention reduced guideline-discordant bone scans among low-risk patients.
- Holding annual academic detailing group sessions on current imaging guidelines may help to sustain the intervention’s effect over time.
Radiographic staging of low-risk prostate cancer is still widely performed, even though clinical guidelines recommend otherwise.
A physician-focused behavioral intervention developed by Danil V. Makarov, MD, together with colleagues at NYU Langone Health, is helping to discourage guideline-discordant imaging in low-risk patients, while emphasizing the importance of imaging for those with high-risk disease. The approach was published in the Journal of the National Cancer Institute.
“Merely publishing clinical guidelines does not change physician behavior.”
Danil V. Makarov, MD
“Contrary to the guidelines, inappropriate imaging to stage low-risk prostate cancer patients is still prevalent,” says Dr. Makarov. “Merely publishing clinical guidelines does not change physician behavior.”
Before routine prostate-specific antigen (PSA) screening, prostate cancer was often diagnosed at an advanced stage, warranting radiographic staging prior to the initiation of treatment. However, since most new diagnoses today are clinically localized, the practice has become obsolete.
In their push for medical resource stewardship, the American Society of Clinical Oncology and the American Urological Association place significant emphasis on reducing the utilization of nuclear medicine bone scanning for early-stage prostate cancer.
A Multimodal, Physician-Centered Intervention
The intervention—Prostate Cancer Imaging Stewardship (PCIS)—combines three evidence-based behavioral strategies to encourage guideline-concordant radiographic staging of incident prostate cancer.
“We designed the intervention to bring about lasting behavioral change.”
Academic detailing, the first strategy, is an initiative designed to educate providers on the imaging guideline recommendations.
The second and third strategies are systems-level interventions. These include reminders integrated into electronic order systems, as well as quarterly audits and feedback on ordering performance, all conducted in accordance with the guidelines.
Testing the Intervention
The stepped-wedge, cluster-randomized trial was conducted at 10 Veterans Health Administration medical centers across the country. A total of 61 urology providers who treat prostate cancer were enrolled, and outcomes were assessed among 2,302 patients with incident prostate cancer.
The researchers found conclusive data supporting the finding that PCIS significantly reduced guideline-discordant bone scans among low-risk patients without negatively affecting required imaging for high-risk patients:
- Among patients who underwent a bone scan in a guideline-discordant manner, 20.4 percent received this imaging during the control period compared with 14.9 percent during intervention (odds ratio=0.54; P=.04).
- Among patients for whom a bone scan was recommended by guidelines but was not performed, 6.8 percent received this guideline-discordant imaging during the control period compared with 5.5 percent during intervention (odds ratio=1.36; P=.36).
Dr. Makarov explains that these data align with earlier work showing high rates of inappropriate imaging among veterans with low-risk prostate cancer.
“We designed the intervention to bring about lasting behavioral change,” Dr. Makarov says, “which could serve as a replicable model across clinical settings.”
A Long-Term Perspective
To further sustain the intervention effect over time, Dr. Makarov recommends providers hold annual academic detailing group sessions on current clinical imaging guidelines.
“Such sessions would provide the dual benefit of reinforcing guidelines to currently enrolled providers and education to newly joined providers,” Dr. Makarov says. “This could be a viable long-term strategy.”